Last Tuesday, a 52-year-old IT professional walked into my clinic in Wakad. “Doctor, my glaucoma treatment is going well, right? My eye pressure is always normal when you check it.”
I looked at his reports. Yes, his daytime pressure readings were perfect. But his visual field test showed the disease was still getting worse.
After some questions, I found out he works night shifts twice a week, sleeps on his stomach with his face pressed into the pillow, and his wife says he snores so loud the neighbours probably hear it.
“Your eyes are under attack at night,” I told him. “And we’ve only been checking what happens during the day.”
As a glaucoma specialist in Pune, I frequently observe this pattern. We focus so much on daytime eye pressure that we forget that your eyes are working 24 hours a day. And for many people, the real damage happens when they’re asleep.
Let me explain what’s actually going on.
Think of your eye like a sink. There’s a tap that keeps adding water (your eye makes a fluid called aqueous humor), and there’s a drain at the bottom (the trabecular meshwork – fancy name for your eye’s drainage system).
When the drain works properly, water flows out as fast as it comes in. Pressure stays normal. Your optic nerve – the cable connecting your eye to your brain – stays healthy.
When the drain gets clogged or slows, pressure builds up. That extra pressure squeezes and damages the optic nerve, bit by bit, day by day. You don’t feel pain. You don’t notice anything at first. Your side vision just quietly disappears.
By the time most people realise something’s wrong, significant damage has already happened. That’s why we call glaucoma the “silent thief of sight.”
And here’s what surprised me even more when I started looking into the research: for many patients, the highest pressure occurs at night.
When you’re sitting in my clinic at 11 AM, I measure your eye pressure. Let’s say it’s 16 mmHg – perfectly normal.
But what about 2 AM when you’re deep asleep? Studies using 24-hour monitoring devices have found that eye pressure can be 3-6 mmHg higher at night, especially when you’re lying flat.
That means the same person with “normal” 16 mmHg pressure during the day might be hitting 20-22 mmHg at night, every single night, for 6-8 hours.
Why does this happen? Two reasons:
First, gravity stops helping you. When you’re upright, gravity pulls fluid down and away from your head. When you lie down, blood and fluid shift toward your head, naturally increasing pressure inside your eyes.
Second, your body’s internal clock affects eye pressure. Your eyes produce fluid and drain it based on circadian rhythms. For many people with glaucoma, this rhythm means more pressure at night.
Here’s the problem: if I only check your pressure during office hours, I’m missing those nighttime spikes. And those spikes, happening every night for months and years, cause real damage to your optic nerve.
Why Glaucoma Gets Worse at Night
|
Last month, I had a patient whose glaucoma kept progressing despite perfect medication compliance. His daytime pressures were significant. His wife accompanied him to the appointment and mentioned, almost casually, “He snores like a freight train, doctor. I’ve moved to the other room.”
That was the clue.
Sleep apnea, when you repeatedly stop breathing during sleep, is a bigger glaucoma risk than most people realise. Studies show that people with sleep apnea have roughly three times higher risk of developing glaucoma. (source)
Here’s why: When you stop breathing, even for just 10-15 seconds:
This happens dozens, sometimes hundreds of times per night. Your optic nerve is being stressed repeatedly, regardless of how well your glaucoma treatment is controlling daytime pressure.
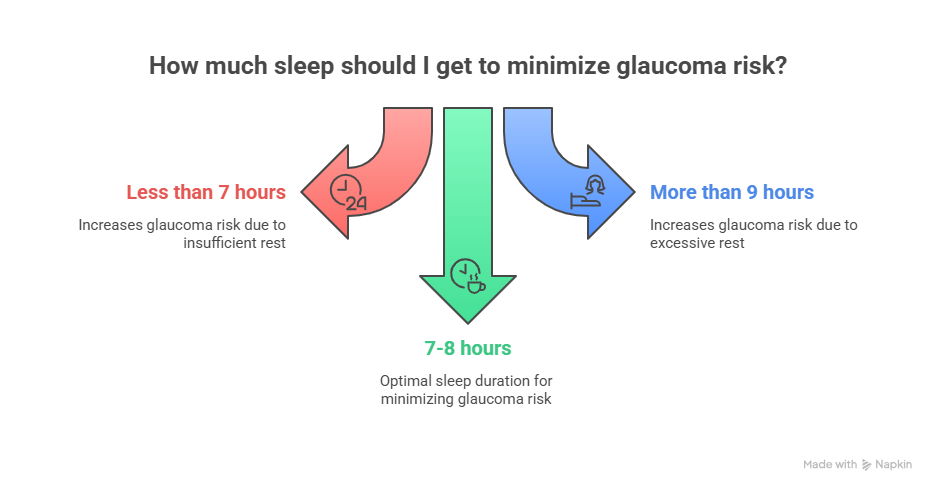
If you snore loudly, wake up gasping for air, or feel tired despite getting 7-8 hours of sleep, please consider getting checked for sleep apnea. Many of my Pune patients work in IT, often experiencing long hours, stress, weight gain, and irregular sleep patterns. Sleep apnea is a common condition that can significantly affect your eyes.
Remember my patient who slept on his stomach? Here’s what was happening:
When you press your face into a pillow – whether you’re a side sleeper or stomach sleeper – you’re putting direct mechanical pressure on your eyeball. Research shows this can increase eye pressure by 2-5 mmHg in the compressed eye. (source)
“Just 2-3 mmHg, doctor? That’s nothing,” patients tell me.
But in glaucoma treatment, we celebrate when medications reduce pressure by 2-3 mmHg. That small reduction can significantly slow disease progression. So adding 2-5 mmHg every night for years? That’s substantial damage.
I’ve noticed a pattern in my practice: patients with worse glaucoma in one eye often sleep on that side. The left eye worse? They sleep on their left side.
Sleep on your back with your head elevated about 20-30 degrees. This means using a wedge pillow or raising the head of your bed.
Research from multiple studies confirms this position:
Yes, changing how you’ve slept for decades is difficult. But if you have glaucoma, this is one of the simplest ways you can protect your vision.
How Sleep Position Affects Eye PressureThe Way You Sleep Matters
| Simple Fix: Raise Your HeadElevate Your Pillow — Protect Your Eyes
|
Let me share some observations from treating hundreds of glaucoma patients here in Pune:
I know, I know – evening tea is sacred. However, caffeine within 3-4 hours of bedtime can increase eye pressure. One cup of coffee can raise your pressure by 1-4 mmHg for several hours.
If you’re having multiple cups in the evening, that’s adding up. Try switching to herbal tea after 5 PM if you have glaucoma.
We Punekars love our late dinners. However, when you eat heavy meals right before bed and then lie down, it increases abdominal pressure, which can, in turn, increase eye pressure.
Try to finish dinner 2-3 hours before going to bed. It is better for your eyes and your digestion.
We’re all guilty – scrolling Instagram, watching one more Netflix episode in bed. Prolonged screen time in the dark can cause your pupils to dilate and disrupt the regulation of eye pressure.
Additionally, blue light disrupts sleep quality, and poor sleep is associated with poorer glaucoma outcomes. Put the phone down at least 30 minutes before bed.
Stay hydrated during the day, absolutely. But chugging a large glass of water right before bed causes a temporary spike in eye pressure. Drink steadily throughout the day, but reduce your intake as bedtime approaches.
Many patients ask me, “Doctor, morning or night?”
If you’re using pressure-lowering drops once daily, taking them before bedtime can be more effective because you’re protecting your eyes during those vulnerable nighttime hours.
However, and this is crucial, every patient is unique. Some medications are more effective at certain times of day. Never change your schedule without consulting your glaucoma specialist.
Additionally, if you take blood pressure medication at night, consult both your physician and your eye doctor. Aggressive nighttime blood pressure lowering, combined with high eye pressure, can reduce blood flow to your optic nerve, which is concerning.
Most glaucoma patients have no symptoms until the late stages. But some warning signs related to sleep include:
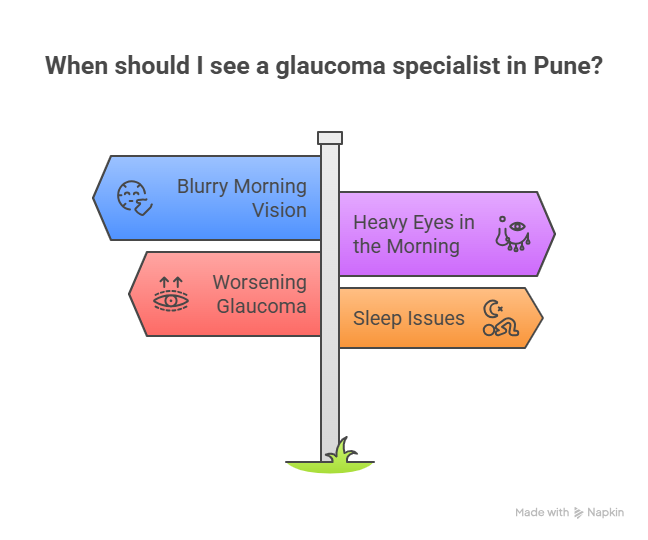
If you notice any of these, come see an eye specialist promptly. With glaucoma, early detection is everything.
You’re at higher risk if you have:
For my Pune patients specifically: if you work night shifts, have irregular sleep schedules, or work in high-stress jobs with poor sleep habits, you’re in a higher risk category. Your body’s natural rhythms affect the regulation of eye pressure.
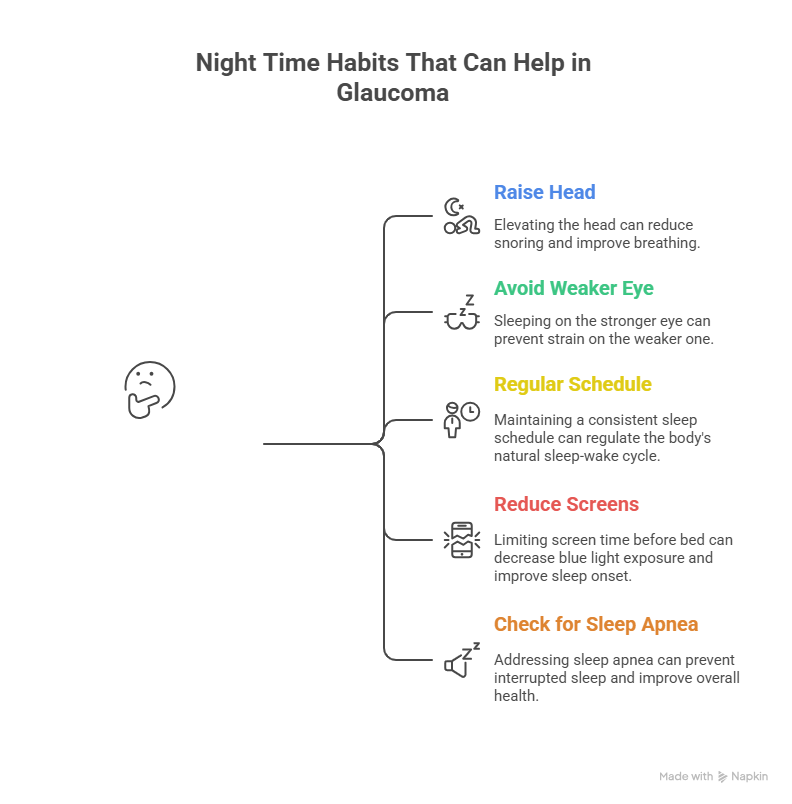
Enough about problems. Here’s what actually helps:
Sleep on your back with your head elevated at a 20-30 degree angle. Use a wedge pillow, not multiple regular pillows (they don’t maintain the angle properly). If you must sleep on your side, alternate sides regularly.
Go to bed and wake up at the same time daily, even on weekends. Your eyes love routine. Your internal pressure rhythms sync better with consistent sleep schedules.
If you snore or your partner complains about your breathing at night, get a sleep study done. Treating sleep apnea can significantly improve outcomes for individuals with glaucoma. Just coordinate with both your sleep doctor and eye doctor about CPAP settings.
Dark, cool room. However, keep a small nightlight if you need to get up at night – sudden exposure to bright light isn’t ideal for your eyes.
Regular exercise is great for glaucoma. But finish vigorous workouts 3-4 hours before bedtime. Morning or afternoon exercise is ideal.
Stay hydrated during the day. After 5 PM, taper off caffeine and large amounts of water.
If you have glaucoma or are at risk, you need regular monitoring. Not once a year – every 3-4 months minimum. These aren’t optional. We need to catch any progression early and adjust your glaucoma treatment before irreversible damage occurs.
Sometimes, despite medication, eye drops, and lifestyle changes, eye pressure remains high or vision continues to deteriorate.
In those cases, we might need to consider surgical options. Modern glaucoma surgeries have improved dramatically – we have minimally invasive procedures that significantly reduce pressure with a quick recovery.
But the goal is always to catch and manage glaucoma early enough that surgery isn’t needed. Prevention beats surgery every time.
Your eyes don’t clock out when you sleep. For many people with glaucoma, nighttime is when their eyes face the most stress.
The good news? You have more control than you think. Simple changes – such as how you sleep, your evening routine, and treating sleep apnea – can genuinely protect your vision.
But you need to act now. Glaucoma is progressive. Once vision is lost, it can’t be restored. What we can do is preserve what you have and prevent further loss.
If you’re over 40, have a family history of glaucoma, or have any of the risk factors I mentioned, get a comprehensive eye exam. Don’t wait until you notice symptoms.
And if you’re already on glaucoma treatment but your condition is still progressing despite good daytime pressure, talk to your eye doctor about 24-hour pressure patterns and sleep-related factors. There might be a nighttime problem we’re missing.
I’m here at Clarity Eye Care in Wakad and Hinjawadi whenever you need me. Let’s protect your vision together – day and night.
Remember: glaucoma might be the “silent thief,” but we don’t have to let it steal your sight quietly.
Book your comprehensive glaucoma screening today. Your future self will thank you.